Learning effective trigger point work can be a seemingly magical component to add to your toolbox of manual therapy skills. Ask any therapist who has been doing precise trigger point work for a length of time and you are likely to hear a plethora of stories of wonderful results that range from the clinically satisfying to the downright miraculous. Here is a recent example from my own practice:
Martha, aged 88, came to me with severe knee pain. Although registered blind and with a severe hearing problem, Martha led an independent lifestyle and loved taking the bus into town to do her own shopping. The knee pain had now been a problem for several months and radially affected her mobility meaning that she could no longer climb stairs easily or walk for longer than about 10 minutes. Convinced that the problem was arthritis, and therefore untreatable, she was completely despondent.
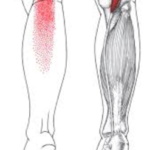
An assessment of the area revealed a multitude of tender trigger points in the quadriceps group, hamstrings, and the smaller muscles that cross the back of the knee – the popliteus and plantaris.(FIG 1 and 2) 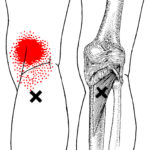
 My treatment approach consisted largely of precise treatment of these trigger points combined with other advanced techniques including fascial work, acupressure and stretching (this successful multi-modal approach is the basis of our book “Massage Fusion: The Jing method for the treatment of chronic pain”). After just one treatment, Martha got off the table declaring herself to feel “80% better”, gave me a big hug and smile and confidently walked down the stairs that she had struggled to get up on the way in. At her next weekly treatment she was able to walk up the stairs easily and was delighted at her increased mobility, declaring it a “miracle”. The second treatment enabled me to work on the 20% of pain still remaining and her third treatment a week later meant that I could ensure these results were long lasting.
My treatment approach consisted largely of precise treatment of these trigger points combined with other advanced techniques including fascial work, acupressure and stretching (this successful multi-modal approach is the basis of our book “Massage Fusion: The Jing method for the treatment of chronic pain”). After just one treatment, Martha got off the table declaring herself to feel “80% better”, gave me a big hug and smile and confidently walked down the stairs that she had struggled to get up on the way in. At her next weekly treatment she was able to walk up the stairs easily and was delighted at her increased mobility, declaring it a “miracle”. The second treatment enabled me to work on the 20% of pain still remaining and her third treatment a week later meant that I could ensure these results were long lasting.
Near instantaneous results like these are surprisingly common with precise trigger point work and the best news is that you don’t have to be an expert with lots of years of practice under your belt to be able to make a radical difference to people’s lives.
So what is a trigger point exactly?
Although the term trigger point has passed into more common usage since the publication of Travell and Simons seminal works in the 80s there is still a surprising amount of mis- information about what trigger points actually are (and aren’t), not to mention the best way to treat them.
Let’s start with the universally known classic definition from Travell and Simons themselves –you will be hard pressed to read an article or book on trigger point therapy without encountering the classic soundbite below
According to “the source”, a trigger point is:
A hyper irritable spot in skeletal muscle that is associated with a hypersensitive palpable nodule in a taut band. The spot is painful on compression and can give rise to characteristic referred pain, referred tenderness and autonomic phenomena.”
Travell and Simons 1999:5
As this definition tends to make a large percentage of the population glaze over, most of your clients are likely to understand trigger points as “muscle knots” ie: lumps and bumps in their muscles that are responsible for their pain. Although the muscle has definitely not tied itself into a knot, clearly the average massage therapist is well aware that clients will be seeking help for relief from these pesky “muscle knots” – a brief google search reveals a plethora of suitably named bodywork businesses including Knotstressed, no more knots, knowyourknots, knots away, bodyknots massage, niggles and knots and knuckles and knots. Clearly the knot analogy is a pervasive image and we all instinctively feel the urge to poke around our own bodies when we are in pain to try and find these “hot spots”.
So if trigger points are not actually knots what are they? The key points about trigger points as drawn out from this definition are:
• They “feel” like knots in muscle but are in fact small areas of tightly contracted muscle (NOT the same as a whole muscle spasm) (FIG 3)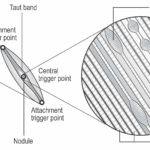
• They are usually found within a taut band of skeletal muscle which can be palpated
• If you press on the trigger point it hurts
• This is the most exciting point to therapists- the pain has a characteristic referred pain pattern. This means that the pain from trigger points often causes pain in other parts of the body distant from the trigger point itself. A good example is trigger points in the SCM muscle that can commonly cause headaches or jaw pain. Or trigger points in the piriformis muscle that can cause a pain down the leg commonly confused with sciatica. Or trigger points in the quadratus lumborum that cause pain around the sacrum that can feel like sacro-iliac pain. (FIG 4)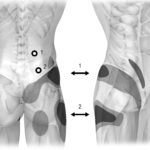
• There is also a lesser known slightly mysterious part to the definition– trigger points can also cause “autonomic referred phenomenon”. In other words trigger points can also cause symptoms you would never guess were coming from your muscles- for example ringing in the ears or dizziness can be caused by trigger points in the SCM.
The concept of referred pain is an important one as it means that the source of the pain can often be in a different location than where the client is feeling their discomfort. This is critical to what we do as massage therapists, as the theory of trigger point therapy suggests that if we are only treating the area of pain we are unlikely to achieve lasting results. It is likely that if the cause is myofascial trigger points and you are only in the area of pain, you will be in the wrong place 75% of the time! (Chaitow and DeLany 2000: 69)
What are the effects of trigger points?
Pain
The bad boys of the body, trigger points are always up to no good. Travell and Simons go so far as to describe them as the “scourge of mankind” (Travell and Simons 1999: 14) Many researchers have corroborated the notion that trigger points are implicated in up to 95% of chronic musculo- skeletal pain (Malaga et al 2010), with one study suggesting that trigger points are the sole cause of such pain as much as 74 % of the time (Gerwin 1995). A study of musculoskeletal disorders in Thailand found that myofascial pain syndrome was the primary diagnosis in 36% of 431 patients with recent onset pain (Chaiamnuay et al 1998)
The pain from trigger points can manifest in many different ways – it can feel dragging, stabbing, dull, tingling, burning, superficial or deep in the joint. Trigger points can also be known to cause weakness in the affected muscles. Because there is a lack of awareness as to the concept of trigger points, the pain is often misdiagnosed as having a more serious or unknown cause leading to unnecessary medical tests or fear and hopelessness on the part of the client.
Compression of nerves and blood vessels
As nerves and blood vessels perforate the muscles at many places, the shortening of muscles caused by trigger points can lead to their entrapment with consequences of numbness, tingling (nerves) or oedema (blood vessels). I have had many cases of misdiagnosed carpal tunnel syndrome in my clinic that have been easily resolved through appropriate trigger point treatment of the scalenes or pectoralis minor, both of which, when shortened by trigger points, can trap the brachial plexus (nerve bundle that runs down the arm).
Restricted movement
The taut bands that arise in connection with trigger points lead to shortening of the muscles – this in turn leads to reduced mobility and potentially joint dysfunction
Autonomic Effects
Autonomic effects can be found both in the area of the trigger point and in the area of referred pain. Autonomic effects include changes to skin temperature, increased sweat secretion, nausea or dizziness. Some other more bizarre cases of autonomic effects cited by Travell and Simons comprise reddening of the eyes, excessive tearing, blurred vision, a droopy eyelid, excessive salivation, persistent nasal secretion and goose bumps.
Adhesions and contractures
Persistent trigger points in muscles can lead to stiff ropy like cords in the muscle – these are caused by fascial adhesions overlying and fixing the trigger point complex. Layers of connective tissue literally stick to each other causing hard, ropy muscles that feel like they are glued together. These are known as adhesions and severe cases can even develop into a form of contracture, similar to that seen in people with paralysis. Adhesions literally “lock in” trigger points making them more difficult to treat and compounding problems of pain and movement. Contractures also affect the overall functioning of the muscle; the contracture is felt as hard, tight and fibrotic whereas the rest of the muscle becomes weak and atrophied. (Chen et al 2006)
Incorporating trigger point therapy into your massage treatments
In the context of the Jing multi- modal approach, precise trigger point therapy is the “meat of the sandwich”– a powerful tool in its own right but even more effective when combined with the other modalities recommended.
At the point of the treatment where you are ready to carry out the precise trigger point techniques you will have already:
• Carried out an outcome oriented consultation that has enabled you to identify potential trigger point activating factors including the role of emotional and psychological factors, beliefs, lifestyle and possible central sensitisation factors
• Applied heat to the body to enhance the effects of fascial and trigger point release
• Applied fascial techniques to release fascial adhesions and broad areas of trigger point activity.
So now you are ready to carry out the precise trigger point protocols that have served us so well in the treatment of pain for many years. Our book “Massage Fusion: The Jing method for the treatment of chronic pain” gives you precise methods to treat pain in different areas of the body but the methods all rely on the same basic trigger point treatment principles as outlined below.
The method of trigger point treatment expounded here is based on principles originally taught by chiropractor Raymond Nimmo, a contemporary of Janet Travell. The approach was known as ‘receptor-tonus’ technique (Nimmo 1957). Nimmo’s work has influenced several well- known manual therapy approaches to trigger point including Paul St John neuromuscular technique and modern American style neuromuscular therapy (DeLany 1999)
The method has a few distinct hallmarks that in our view make the technique highly effective and more importantly, easy to learn:
• The method relies on treating all the muscles around the affected joint for trigger points. In this way, the practitioner is using a precise approach that logically examines all the muscles that may contain both key and satellite trigger points. The therapist does not have to rely on interpreting complicated trigger point diagrams to trace back the source of the client’s pain. This massively simplifies the therapist’s ability to obtain effective results with common musculo-skeletal pain. So for example to treat low back pain, the therapist searches for trigger points in the erector spinae, quadratus lumborum, gluteus maximus, gluteus medius, hamstrings and psoas. This is a bit of a “no brainer” approach to trigger point treatment that is simple to learn and has effective results.
• To accurately identify trigger points, the therapist palpates the full length of the muscle being treated encouraging precise communication from the client to give feedback on any points that reproduce their primary pain complaint.(FIG 5) This helps to reduce one of the most common reasons for trigger point treatment failing to work – namely the inability of the therapist to find them! Engaging the client in the process enables the practitioner to develop their sense of “listening touch” and gain appropriate feedback about what they “think” they feel. This eventually also builds confidence and palpation skills on the behalf of the therapist.
This helps to reduce one of the most common reasons for trigger point treatment failing to work – namely the inability of the therapist to find them! Engaging the client in the process enables the practitioner to develop their sense of “listening touch” and gain appropriate feedback about what they “think” they feel. This eventually also builds confidence and palpation skills on the behalf of the therapist.
• Key trigger points (those that reproduce the client’s pain) are treated with static compression for between 8-12 seconds again engaging with the client about the nature of the pain. Key trigger points may be treated up to 3 times in a session.
• The key trigger points are treated in a similar manner (by following the same routine of treating all the muscles around the joint) on a weekly basis for up to 6 weeks. Generally a decrease in pain is noted at the latest around the third weekly session at which point the time between treatments is lengthened (ie: to once every 2 weeks).
What do trigger points feel like?
Some trigger points are tiny almost like a grain of rice whereas others can feel like a pea or even walnut sized. They are usually found within a tighter bit of muscle (the taut band) When you first start to do this work it is likely you will have no idea what a trigger point feels like which is why it is crucially important to work with client communication. Over time your palpation skills will develop and you may eventually feel so confident in your ability to locate them that the client feedback can become more minimal.
Communication skills in trigger point work
Good communication with your client is crucial when doing trigger point work. Agreed verbal or non verbal feedback from your client will let you know whether you have located the trigger point accurately. It is important to educate your client as to your need for them to communicate during the treatment, as this is not something we would usually encourage during a pure relaxation massage.
Explain to your client during the consultation that you will be looking for “hot spots” in their muscles that reproduce the symptoms they are experiencing. When you find one it is important that they let you know either verbally or via a prearranged non verbal signal ie: wiggling the fingers of the right hand (this can be important as when your client is prone it is impossible to decipher the mumblings into their face cradle. A few frustrating rounds of “is that something?” “mwh mwh mwh” is enough to raise both yours and your client’s trigger point activity by itself!)
Communication can be kept to a minimum but you will need to know:
• Is the spot tender?
• Is there any referred pain when pressing on the point?
• On a pain scale of 1-10 (1 being no pain, 10 being the most) where would they rate their “good hurt” from the pressure. Your pressure should NEVER be causing a pain that is above a 6 on the pain scale – if it is then ease up. More pain does NOT mean more gain.
• After 8 -12 seconds of pressure has the pain released and diminished?
To get the best therapeutic results from your work it is important not to cause the person pain. You must always use a pressure that is beneath the client’s pain threshold. I usually say to my clients ” if you feel like clenching your fists or teeth while I am treating you please let me know and I will ease off the pressure”
In summary
I feel indebted to the discovery of precise trigger point work as without a doubt it has enabled me to achieve long lasting results in the treatment of thousands of chronic pain conditions. I would urge you to find out more about this fascinating technique as it will not only enhance your results but boost your practice.
About Rachel Fairweather and Jing Advanced Massage
Rachel Fairweather is author of the best selling book for passionate massage therapists – ‘Massage Fusion: The Jing Method for the treatment of chronic pain”.
She is also the dynamic co-founder and Director of Jing Advanced Massage Training (www.jingmassage.com), a company providing degree level, hands-on and online training for all who are passionate about massage. Come and take part in one of our fun and informative short CPD courses to check out the Jing vibe for yourself!
Rachel has over 25 years experience in the industry working as an advanced therapist and trainer, first in New York and now throughout the UK. Due to her extensive experience, undeniable passion and intense dedication, Rachel is a sought after international guest lecturer, writes regularly for professional trade magazines, and has twice received awards for outstanding achievement in her field.
Rachel holds a degree in Psychology, a Postgraduate Diploma in Social Work, an AOS in Massage Therapy and is a New York licensed massage therapist.
www.jingmassage.com
Tel: 01273 628942
Copyright Jing Advanced Massage July 2019.



Comments are closed.